What causes LGS?

In LGS, the brain is affected at a critical time in its development. Learning problems and seizures result.
There are many causes of seizures that can evolve into LGS. While we don’t know why seizures evolve into LGS, we do know that finding the cause of seizures requires extensive testing. In some cases, more than one cause may be found.
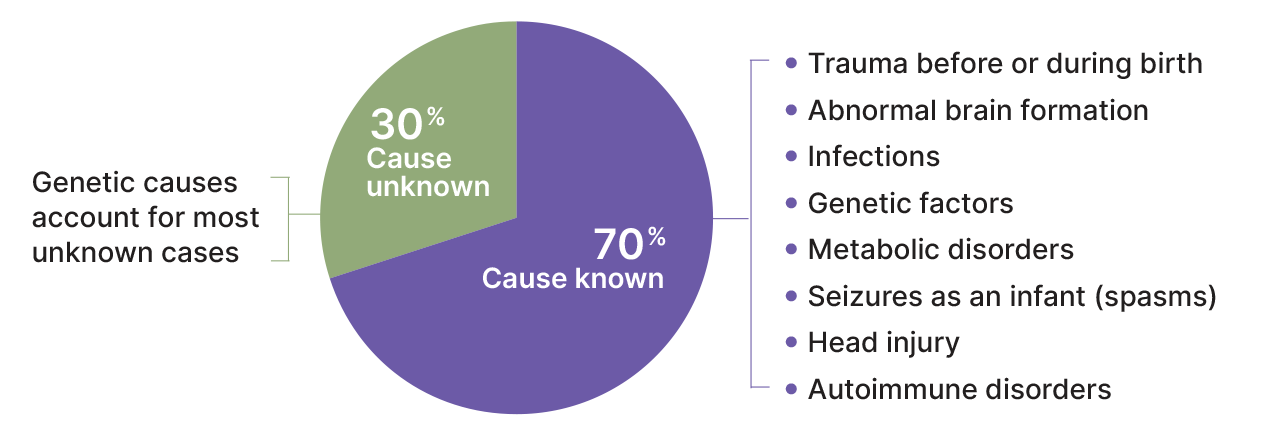
Causes of LGS may include:
- Infection during pregnancy
- Genetic abnormality
- Low oxygen or blood flow to the brain (e.g. Hypoxic Ischemia or HIE)
- Brain infection (e.g. meningitis, encephalitis)
- Traumatic brain injury (e.g. stroke)
- Early brain radiation
- A lack of essential nutrients to keep brain cells healthy
- A toxic buildup that results in brain cell dysfunction
- Prenatal infection. Viruses can infect the fetus during pregnancy. Blood tests and eye exams can usually detect prenatal infection.
- Brain infection early in life. Brain infections can lead to brain injury and a severe seizure disorder like LGS.
Is the MRI normal in those with LGS?
About 2 out of 3 of those with LGS have abnormal brain imaging at the time of diagnosis. Having an abnormal MRI is often associated with a poorer LGS outcome.
Can LGS evolve from other epilepsy syndromes?
Yes, LGS can also develop from other epilepsy syndromes such as West Syndrome, Tuberous Sclerosis Complex, and Ohtahara Syndrome.
The risk factors for developing LGS include:
- Early life seizures that are treatment-resistant
- Structural abnormalities are seen on the MRI
- Brain injuries at birth or in early childhood (e.g., lack of oxygen, stroke, tumors)
- Mutations in any of the more than 150 epilepsy-related genes (e.g., TSC1, SCN2A, SCN1A, CDKL5, Dup15q, Trisomy 21, FOXG1 Dup, SIK1, GRIN2A, and many more)
- Infantile spasms
- The presence of more than one seizure type
- Epileptic encephalopathy syndromes such as West, Ohtahara, etc.
- Developmental slowing or regression
- Failure of >2 anti-seizure treatments
Having all of these risk factors does not mean someone will develop LGS. It means they are at high risk of developing LGS. We do not know why some with these risk factors develop LGS, and some do not.
Watch: Causes of LGS and What They Mean
2019 LGS Foundation Family Conference in Seattle, Washington, Tracy Dixon Salazar, Ph.D. – CAUSES OF LGS AND WHAT THEY MEAN
 Thank you to the Child Neurology Foundation for allowing us to adapt this article for this site. Authors: Shaun Ajinkya, MD; Elaine Wirrell, MD, Mayo Clinic – Rochester, Minnesota Reviewed: April 2021
Thank you to the Child Neurology Foundation for allowing us to adapt this article for this site. Authors: Shaun Ajinkya, MD; Elaine Wirrell, MD, Mayo Clinic – Rochester, Minnesota Reviewed: April 2021
The information here is not intended to provide diagnosis, treatment, or medical advice and should not be considered a substitute for advice from a healthcare professional. The content provided is for informational purposes only. LGSF is not responsible for actions taken based on the information included on this webpage. Please consult with a physician or other healthcare professional regarding any medical or health related diagnosis or treatment options.
Updated 7/11/2023
